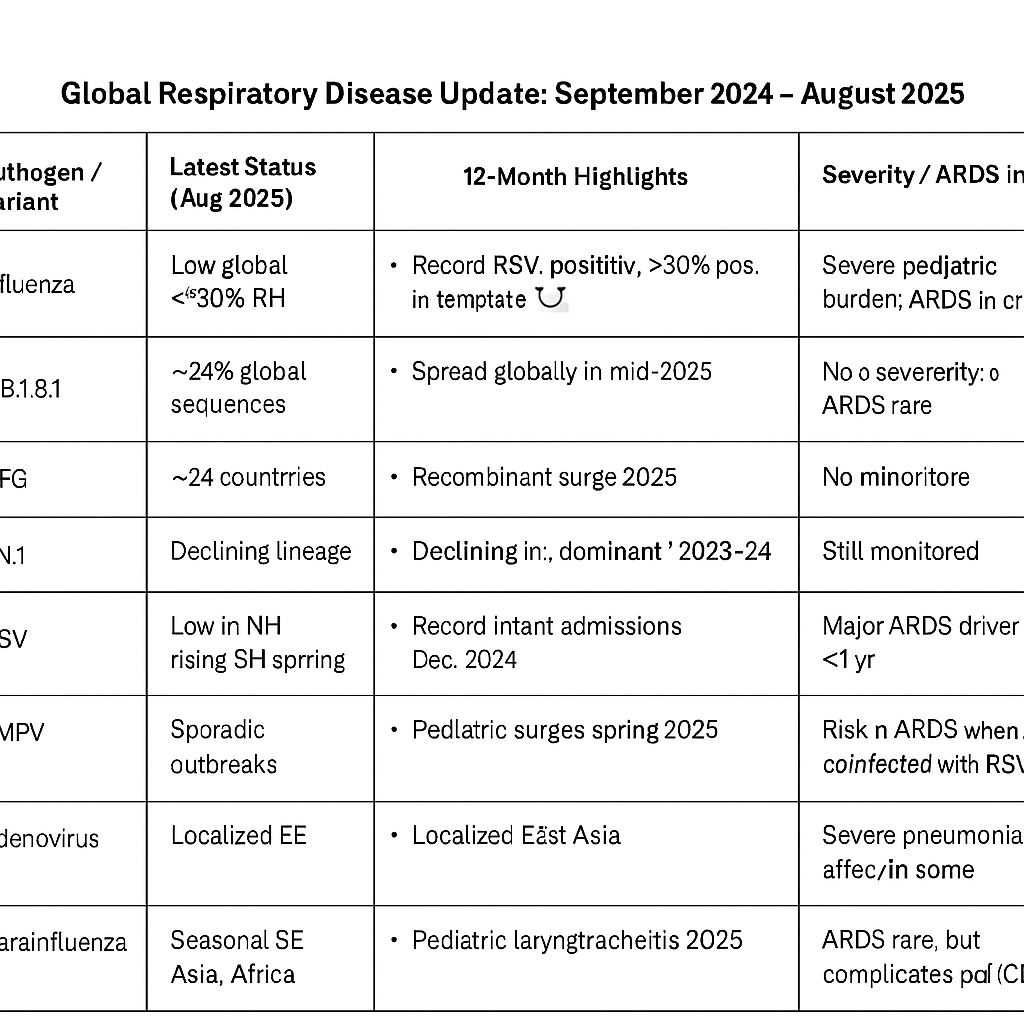
🌍 At a Glance
The past 12 months have seen shifting patterns in respiratory pathogens worldwide:
Influenza activity followed seasonal cycles, peaking Jan–Feb in the Northern Hemisphere. COVID-19 variants NB.1.8.1 (“Nimbus”), XFG (“Stratus”), and residual JN.1 (“Pirola”) altered genomic landscapes without increasing severity. RSV (Respiratory Syncytial Virus) drove record infant hospitalizations in the 2024–25 NH winter, but new maternal vaccines and monoclonal antibodies changed prevention strategies. Other acute respiratory distress syndrome (ARDS) drivers (adenovirus, hMPV, parainfluenza) contributed to localized pediatric outbreaks and coinfections.
🦠 Influenza (Sep 2024 → Aug 2025)
Northern Hemisphere: Peaked late Jan / early Feb 2025; pediatric deaths in the U.S. reached 270 — a record for non-pandemic years. Summer 2025: Low baseline across most temperate zones, but >30% positivity in parts of Central America/Caribbean, Africa, and SE Asia. Circulating strains: A(H1N1)pdm09, A(H3N2), and B/Victoria co-circulated in Europe.
🧬 COVID-19 Variant Dynamics
NB.1.8.1 (“Nimbus”): ~24% of global sequences by June 2025; faster transmission, no severity increase. XFG (“Stratus”): Recombinant variant in 38 countries; ~30% UK, ~14% U.S. detections. JN.1 (“Pirola”): Once dominant (2023–24), now receding but under monitoring. Public health impact: No vaccine-escape evidence; WHO classifies all as Variants Under Monitoring.
👶 RSV (Respiratory Syncytial Virus)
2024–25 NH winter: Record RSV admissions in infants <6 months across U.S., Canada, EU. CDC reported RSV hospitalization rates exceeding influenza at the Dec 2024 peak. Countermeasures: WHO issued new position paper (May 2025) on infant protection via maternal RSV vaccination and nirsevimab monoclonal antibody. By summer 2025, rollout underway in multiple high-income countries; access limited in low-income settings. Trend now (Aug 2025): RSV activity very low in temperate NH, but rising in southern hemisphere spring (esp. Argentina, South Africa, Australia).
🧩 Other ARDS-Related Respiratory Viruses
hMPV (human metapneumovirus): Co-circulation with RSV in U.S. spring 2025 caused pediatric bronchiolitis surges. Adenovirus outbreaks: Reported in schools/military in East Asia (winter 2024–25). Some cases complicated by pneumonia → ARDS. Parainfluenza: Seasonal spikes noted in Southeast Asia and sub-Saharan Africa; mostly pediatric laryngotracheitis/ARDS. Coinfection patterns: Increasing use of multiplex PCR panels revealed influenza/RSV or RSV/hMPV dual infections, associated with higher ARDS severity.
🧭 Interpretation Key
High activity + pediatric admissions = major ARDS driver (RSV, hMPV, adenovirus). Novel variants without ↑ severity (COVID-19 NB.1.8.1, XFG) require genomic vigilance but not emergency escalation. Coinfections are increasingly recognized and may double ARDS risk in hospitalized children.
✅ Sources
WHO Influenza Update N° 541 (Aug 2025) CDC FluView Weekly Reports (Aug 2025) ECDC ERVISS (Aug 2025) WHO RSV Position Paper (May 2025) PAHO Epidemiological Bulletins Scientific reporting (Time, Guardian, peer-reviewed updates on NB.1.8.1 / XFG / JN.1) ChatGPT (OpenAI Assistant) — synthesis and narrative construction based on cited sources.
🔍 SEO Metadata
Meta Title: Global Respiratory Disease Report (2024–25): Influenza, RSV, COVID-19 Variants & ARDS Drivers
Meta Description: The past year saw major influenza peaks, record RSV infant admissions, and new COVID-19 variants NB.1.8.1 & XFG. Review the latest WHO/CDC/ECDC data on respiratory and ARDS trends.
Slug: /global-respiratory-disease-update-2024-2025